
New Walgreens medication management app. Image credit: www.patentlyapple.com
Medication Non Adherence (MNA)
The risk to patients’ health and cost to the healthcare system associated with MNA are both well documented. Most studies now estimate that approximately 50% of all patients do not take their medication correctly and that in the US alone, MNA costs the healthcare payers about $300bn.
Good adherence is particularly difficult for people whose treatment regimens may be more complex and involve a number of medicines to be taken each day. Typically this includes patients with a long-term conditions, such as diabetes, cancer, heart disease and multiple sclerosis.
Mental health
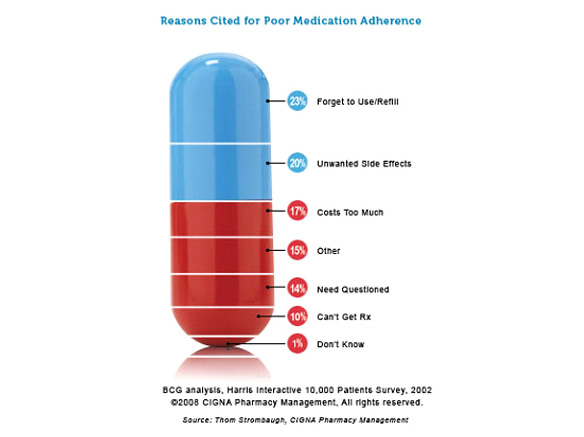
In numerous studies, patients often cite forgetting to take medications or refilling their prescriptions as the main reason behind MNA. However, as the figure above illustrates, there are a variety of ‘other’ reasons why people do not take their medications correctly. Among these less talked about ‘other’ factors are depression and (to a lesser degree) anxiety disorders – mental health problems that are commonly experienced by a large number of people on long-term medication regimens.
Unfortunately, anxiety and depression are two of the most common mental health concerns in developed societies, with anxiety reported in 1 in 13 globally and depression about 1 in 20.
In chronic disease sufferers, US data shows that depression is prevalent in 17 percent of cardiovascular cases, 23 percent of cerebrovascular cases and 27 percent of diabetes patients. For cancer patients, the number is 40 percent. As one-to-one treatment for common mental health problems can be out-of-reach – financially and/or geographically – many sufferers do not have access to professional therapists. It’s no wonder, then, that we are seeing an increasing number of apps and devices targeting depression and mood management. In this post, we take a look at a couple of digital tools that aim to make a difference in this area.
Wearable that targets depression
The SunSprite wearable light tracker by Boston start-up, Goodlux Technology, is the first wearable device to track daily bright light intake in an attempt to control depression. According to GoodLux, scientific studies have linked bright light exposure to health benefits such as better energy, mood and sleep, and can improve the efficacy of broader care plans for patients with depression and chronic diseases. A solar powered device that clips onto clothes and connects to a mobile app, SunSprite contains sensors that measure visible and UV light and indicates to users when they’ve absorbed enough sunlight to maintain health.
![]()
Online therapy for social anxiety
Starting with a 12-week programme of cognitive behavioural therapy (CBT) to help overcome social anxiety, Joyable is an online mental health service provider that is on a mission to cure the world of anxiety and depression. According to Joyable CEO, Peter Shalek “CBT is the most effective treatment for social anxiety, bar none – it’s more effective than medication and more effective than other forms of therapy.” Research studies and health providers, including the NHS, have also found that CBT via the internet can be just as effective as face-to-face therapy with a therapist for mental health problems.
Along with a tailored online program, for $99 per month Joyable provides activities designed to reduce social anxiety and a dedicated coach, a ‘real’ person who is, in fact, credited for helping clients stick with the program. The success of Joyable (the founders claim 90% of their clients experience a reduction in their social anxiety) is testament to the fact that for sustained user-engagement the human touch is an integral factor.
Human interaction is especially important for patient medication adherence, where good communication and trust between a patient and their healthcare provider(s) is empirically linked to positive outcomes in adherence to prescribed therapy and overall patient satisfaction. At the same time, there is only so much a provider can do to improve adherence in a clinical setting. And this is precisely where digital technology – wearable or otherwise – can play a critical role.
Conclusion
The two examples above show how digital tools can be used to improve the mental state of patients, which has a positive and proven impact on medication adherence. As these types of solutions mature and more choices become available, there is little doubt that they ought to be part of the treatment “toolkit” used by healthcare providers and patients to improve adherence, helping to raise patient wellbeing, optimise healthcare outcomes and reduce cost of medical care.


